Çene Eklemi rahatsızlıkları (TME Hastalıkları)
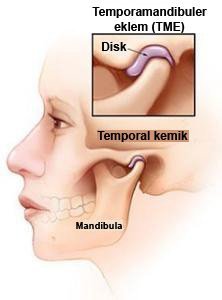 Eklem bölgesinde ağrı veya eklemde fonksiyon bozukluğu olan kişilerin sayısı düşünüldüğünden çok daha fazladır. Eklemin dışındaki komşu yapılardaki değişiklikler ve sistemik hastalıklarda çeşitli klinik bulguların ortaya çıkmasına sebep olur. Bazen kaslarla ilgili bozukluk görüldüğünde ağrı ve fonksiyon kaybı görülebilir.
Eklem bölgesinde ağrı veya eklemde fonksiyon bozukluğu olan kişilerin sayısı düşünüldüğünden çok daha fazladır. Eklemin dışındaki komşu yapılardaki değişiklikler ve sistemik hastalıklarda çeşitli klinik bulguların ortaya çıkmasına sebep olur. Bazen kaslarla ilgili bozukluk görüldüğünde ağrı ve fonksiyon kaybı görülebilir.
Temporamandibuler Eklem Bozuklukları
Temporomandibular bozukluklar Temporomandibular Eklem (TME) ve\veya çiğneme kaslarını tutan ağrı ve disfonksiyon sendromudur.
TME bozukluklarının semptomları
- Kulaklarda çınlama
- Ağzınızı açıp kapatırken gıcırdama, klik, takırtı sesi
- Çenenizi limitli açma veya kilitlenme
- Boyunda ağrı veya sertlik
- Baş dönmesi, bayılma
- Çiğnerken ağrı
- Yüzde ağrı
- Dişleri birbiri üstüne kapatırken ağrı
- Çiğnerken çenede yorgunluk
- Ellerde uyuşukluk
- Esnemede zorluk
TME’de diskin deplasmanı yada kondil ve diskte dejeneratif değişiklikler de oluşabilir. TME’deki klinik semptomlardaki farklılıklar her zaman disk deplasmanı olarak açıklanamaz. Çiğneme kaslarının fonksiyonu ve disfonksiyonu da hesaba katılmalıdır.
Temporamandibuler Eklem Bozukluklarına Sebep Olan Faktörler
- Çenelere gelen direkt travma (kaza yada darbe sonucu),
- Diş yada medikal tedavi sırasında oluşan iatrojenik(hekim kaynaklı) yaralanmalar,
- Eklemin gelişimsel defektleri( hipoplaziler vs.),
- Dejeneratif eklem rahatsızlıkları,osteoartritis,artrozis,
- Otoimmün hastalıklar, romatoid artrit, lupus,
- Parafonksiyonel çene aktiviteleri: gıcırdatma, bruksizm,
- Orofasiyal hareket bozuklukları,
- Davranışsal bozukluklar: stres,depresyon,somatizasyon,
- Çene ilişkilerindeki major uyumsuzluklar,
- Dental okluzyondaki major uyumsuzluklar,
- Bilinmeyen faktörler.
TME Rahatsızlığımı Nereden Anlarım?
- Sıra dışı bir ağrınız oldu mu?
- Çenenizi açıp kapattığınızda tıkırtı,klik yada tak diye bir ses geliyor mu?
- Bu bölgelerde ağrı veya sızınız var mı? Çene eklemleri, alt çene, üst çene, boyun, başınızın arkası, alın, şakaklar.
- Kulağınızda tıkanıklık, basınç veya aşırı kir salgılama oluyor mu?
- Kulağınızda çınlama, gürleme gibi sesler oluşuyor mu?
- Daha önce baş dönmesi hissettiniz mi?
- Ellerinizde, parmaklarınızda veya kollarınızda ürperti veya uyuşma oluyor mu?
- Her zaman kolayca yoruluyor musunuz yada kronik yorgunluğunuzun olduğunu düşündünüz mü?
- Dilinizin olduğu tarafta dişlerinizin izi oluşuyor mu?
- Yutkunduğunuzda diliniz dişlerinizin arasına giriyor mu?
- Yemekleri çiğnerken zorlanıyor musunuz?
- Arka bölgede diş kaybınız oldu mu?
- Gece veya gün boyu dişlerinizi sıkıyor musunuz?
- Gece uyurken dişleriniz gıcırdatıyor musunuz? (Ailenize sorun)
- Hiç diş ağrısıyla uyandınız mı?
- Daha önce boyun zedelenmesi yaşadınız mı?
- Daha önce çenenize,yüzünüze veya başınıza bir darbe aldınız mı?
- İlaçların ağrınıza uzun süre etki etmediği oldu mu?
- Çiğneme sırasında semptomlarınız daha da kötüleşiyor mu?
- Parmaklarınızı kulaklarınızın içine götürüp bastırırken ağzınızı açıp kapattığınızda ağrı oluyor mu?
- Çeneniz, ağzınızı açarken sağa yada sola kayıyor mu?
- Ağzınızı açtığınızda ilk 3 parmağınız dik olarak içeri girebiliyor mu?
- Yüzünüzde asimetri var mı?
Eğer bu sorulardan bir çoğuna cevabınız “Evet”se TME hastalığınız olabilir. Diş hekiminize danışmanız gerekir.
Çene Ekleminizi Kontrol Edebileceğiniz Yönetmler
Parmaklarınızı kulaklarınızın içine götürün, birkaç kez çenenizi açıp kapayın. Klik,tıkırtı gibi sesler hissediyor musunuz?
Aynanın karşısına geçin ve çenenizi yavaşça açıp kapayın. Açarken diğer tarafa kayma veya ağrı oluyor mu?
Çenenizi bir taraftan diğer tarafa kaydırın ve ağrı varsa not edin.
Kaslarınızın Hassasiyetini Kontrol Edin:
Parmaklarınızı kulaklarınızın biraz önünde olan eklemlerinizin olduğu bölgeye yerleştirin yanak bölgenize basınç uygulayın.
Herhangi bir rahatsızlık ya da çene ekleminizde ağrı hissediyorsanız TME konusunda uzmanlaşmış bir diş hekimine danışın.
 TME Tedavisi
TME Tedavisi
- Semptomların tedavisi
- Altta yatan nedenin tedavisi
- Predispozan faktörlerin tedavisi
- Patolojik etkilerin tedavisi
Tedavi Seçenekleri
- Hasta eğitimi ve koruyucu
 tedavi
tedavi - Fizyoterapi
- İlaç tedavisi
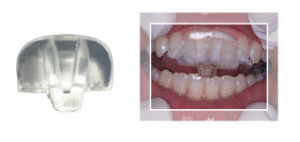
- Splint tedavisi(Gece Plakları,NTİ-tss tedavisi)
- İntra-artiküler enjeksiyonlar (Steroid, Na Hyaluronat vb) ve lavaj
- Genel anestezi altında manuplasyon
- Cerrahi (artroskopik cerrahi, artrosentez, diskektomi, disk tamiri vb.)
- İleri tedavi (romatolojik, endokrinolojik, kulak burun boğaz şikayetleri, psikiatrik destek tedavisi vb.)
