Horlama ve Uyku Apnesi
Horlama
Halk arasında uyku sırasında bireyin çıkarttığı gürültülü ses olarak tanımlanan, tıbsal manası ise özellikle erişkinlerde gözlenen horlamanın en sık nedeni yumuşak damak ve küçük dilin normalden fazla büyümesi ve sarkması ve bu kasların gerginliklerini kaybederek uyku sırasında solunum yolunu tıkaması ve küçük dilin titreşmesidir. Fakat burundan, ses tellerine kadar üst hava yolunu daraltan bütün problemler (alerjik nezle, burun kemiğindeki eğrilikler, sinüzit, alt ve üst çenedeki yapısal anormallikler, dilin aşırı büyük olması) horlamaya sebep olabilir.
Çocuklardaki horlama sıklıkla geniz bademciğinin belirtisidir. Bütün horlamalar hava yolundaki daralmanın göstergesidir. Eğer daralma çok ciddi ise, hava yolu tamamen kapanabilir. Bu da uykuda solunum duraklaması ile sonuçlanır.
 Uyku Apnesi
Uyku Apnesi
Kadınların % 6’sını, erkeklerin % 12’sini etkileyen yaygın bir hastalıktır. Uykuda solunumun (ağızdan ve burundan hava geçişinin) belli sürelerle ve sıklıkla istemsiz olarak durmasıdır. Kişi uyurken, solunum ara ara durup, tekrar başlaması ile kendini gösterir; sıklıkla da şiddetli horlama ile beraberdir. Solunum durması saatte 5 den fazla veya uzun süreli ise, kalp ve beyin başta olmak üzere, vücudun pek çok sistemi olumsuz etkilenir.
Sağlıklı bireyde solunum yolu açık iken apneli hastada yumuşak damak (4) sarkarak uyku esnasında solunum yolunu tıkar.
Hormala ve Uyku Apnesi Kimlerde Daha Çok Gözlenir?
- Kilo fazlalığı. Boyunun kısa ve kalın olması boğazda hava yolunun daralmasına neden olur. Kilo fazlalığı nedeniyle boynun ve boğaz çevresindeki yağ dokusunun artması uyku apnesini şiddetlendiren önemli bir etkendir. Boyun çevresinin, yani gömlek yakası numarasının erkeklerde 43 cm’den, kadınlarda 40 cm’den fazla olması uyku apnesi için risklidir. Ancak uyku apnesi zayıf kişilerde de görülebilir.
- Büyümüş bademcikler ve geniz eti varlığı. Bademciklerin normalden büyük olması ve geniz eti bulunması daha çok çocuklarda görülen uyku apnesinin nedenidir; ancak bazen erişkinlerde de sorumlu olabilir.
- Boğazın dar yapıda olması. Bazı kişilerde boğazın şekli doğuştan dar yapıda olabilir.
- Erkek cinsiyet. Uyku apnesi erkeklerde kadınlardan iki kat sık görülür. Ancak, kilo fazlası olan kadınlarda da sık görülmektedir.
- Yaş. Uyku apnesi orta yaş üzerindeki erişkinlerde gençlere göre 2-3 kat daha sıktır.
- Alkol, sakinleştirici ve uyku ilaçlarının kullanımı. Bu maddeler boğaz kaslarının uyku sırasında gevşemesine neden olurlar.
Horlama ve Uyku Apnesinin Belirtileri
- Şiddetli horlama
- Sabah baş ağrısı
- Kalp şikayetleri ve yüksek tansiyon
- Aşırı ve hızlı kilo alma
- Psikolojik sorunlar, depresyon, cinsel isteksizlik
- Konsantrasyon güçlüğü
- Uykuda aşırı terleme
- Uykusuzluk, gün içinde sürekli yorgun olma
- Sık idrara çıkma, vücudun su kaybetmesi
- Düzensiz ve konforsuz uyku
- Gündüz uyuklama
- Uyku sırasında solunum duraklamasının başkaları tarafından gözlenmesi
- Solunum güçlüğü ile uyanma
- Ağız kuruluğu ve boğaz ağrısı ile uyanma
Horlama ve Uyku Apnesi Ciddi Bir Hastalıktır!
- Acil tedavi gerektiren hayati bir hastalıktır,
- Uykusuzluk, en sık bildirilen uyku şikayeti ve ağrıdan sonra en çok bildirilen ikinci genel şikayettir . NIMH 1984 raporuna göre toplumun %35’ i şikayetcidir ve önemli kalp krizi ve ölüm nedenidir. Amerikan toplumuna tıbbi gider, kaza kayıpları, işe gelmeme kaybı ve üretimde azalmalara neden olmaktadır
- İş yerinde konsantrasyon güçlüğü çektiklerinden yeterince verimli olamazlar ve işlerini kaybetme riskiyle karşı karşıya kalabilirler.
- En tehlikelisi de trafikte araç kullanırken yaşanan problemlerdir. Bu kişiler uyumadan uzun süre araç kullanamazlar. Özellikle akşam üstü ve gece araba kullanırken büyük sıkıntı çekerler. Trafik kazalarının nedenlerinin başında direksiyon başında uyuklama gelmektedir.
Horlama ve Uyku Apnesinin Tedavisi
- Cerrahi Tedavi: Yumuşak damağa yönelik cerrahi müdahaleyi içerir. 1 yıl sonra tekrar nüks etme ihtimali %50’dir.
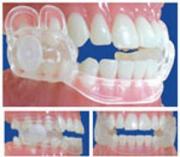
- Cerrahi Olmayan Tedavi: Her gün geceleri 6 saat süreyle takmak şartıyla takılıp çıkarılabilen her bireye özgü olarak hazırlanan özel bir ağız içi protezleriyle ( horlama protezi) kalıcı olarak tedavi edilebilir. Başarı şansı %95’dir.
Horlama Protezitle Horlama ve Uyku Apnesi Nasıl Tedavi Edilir?
Uyku esnasında takılan horlama protezi, gerginliklerini kaybetmiş ve sarkmış yutak bölgesindeki kaslardandolayı tıkanmış solunum yolunu alt çeneye uygun bir konum vererek açar ve horlama ve uyku apnesi engeller.Gerginlkilerini kaybetmiş olan kaslar tekrar eski güçlerine ulaşarak solunum yolundaki tıkanma ortadan kalkar ve horlama ve uyku apnesi kalıcı olarak tedavi edilir.
Horlama Protezinin Diğer Tedavi Yöntemlerine Göre Avantajları
- Cerrahi müdahale içermeden uygulanması
- Cerrahi müdahaleyi reddeden hastalarda alternatif bir tedavi seçeneği olması
- Diğer tedavi seçeneklerine göre iyileşme belirtilerin daha çabuk görülmesi
- Etkinliğinin kanıtlanmış olması
- Çok kısa sürede hazırlanması
- Hastalar tarafından kolayca tolere edilmesi
- Kalıcı olarak tedavi etmesi
Sıkça Sorulan Sorular
Protez geceleri mi takılıyor, rahatsızlık veriyor mu?
Evet, sadece geceleri uyurken kullanılıyor, en az 6 saat takılıyor. Rahatsızlık vermiyor aksine geceleyin uyurken horlamayı ve tıkanmayı engellediği için kişi daha rahat nefes alıyor ve daha konforlu uyumasını sağlıyor.
Ne kadar sürede tedavi olunuyor?
Tedavi süresi hastalığın şiddetine ve hastanın özelliklerine (kilo, yaş, sistemik rahatsızlıklar, cinsiyet v.b.) göre değişmekle beraber ortalama 4-12 ay arasındadır. Kesin süreye klinik muayeneden sonra karar verilebilir.
Protez boğaza kadar mı uzanıyor?
Hayır, sadece dişler üzerine oturarak dişlerden destek anlıyor. Bundan dolayı kullanımı rahat.
Takılıp çıkartılması zor mu?
Hayır, her bireye özgü olarak hazırlandığı için kullanımı çok rahattır, adeta bir gözlüğü takıp çıkarmak kadar basittir.
Geceleyin protez ağzımdayken ağzım açık mı kalacak, ağız kuruluğu yapar mı?
Hayır, dudaklar protez ağızdayken kapanacaktır ayrıca vücuttaki oksijen miktarı yükseleceği için tükürük salgısı normale dönecek ve ağız kuruluğu olmayacaktır.
Protez ne kadar sürede etki edecek?
Kullanılmaya başladığı ilk geceden itibaren etki göstermeye başlıyacaktır, horlama ve tıkanmaların sayısı ilk geceden itibaren azalacaktır (çoğu zaman tamamen kesilir) ve ana etkiler 3-4 hafta içinde gözlenir.
Kullanımı rahat mıdır?
Bireyin kendi ağız yapısına göre hazırlandığı için kullanımı rahattır, bir gözlük ne kadar rahatsızlık veriyorsa protezde o kadar rahatsızlık verir.
Protez malzeme olarak sert midir?
Tedavi etkinliğin artması için sert malzemeden imal edilmiştir. Fakat protezin sert malzemeden yapılması protezin kullanımı açısından güçlük yaratmaz.
Tam dişsizlik durumunda yada ağızdaki herhangi bir protez varlığında da horlama protezi uygulanabilir mi?
Horlama protezi bireye özgü yapıldığı için yukarıda sayılan tüm durumlarda kolaylıkla ve sağlıkla uygulanır.
